-
Birth Brain Injuries
Posted on January 2nd, 2016 No commentsBirth Brain Injuries
1. What is a ‘normal’ birth?
Figures given in ‘ESSENTIAL OBSTETRICS & GYNAECOLOGY’ (E.O.G.) Chapter 17, indicate that 6.7% of live births in England & Wales are Low Birth Weight i.e. less than 2.5 kilograms.
From the same chapter we are told that the common causes of death in the 1st 4 weeks of life are;
1. Major congenital abnormalities incompatible with life.
2. Prematurity- the most important single factor in causing neonatal death, associated with,
a. Respiratory Distress Syndrome.
b. Pnuemonia.
c. Intercranial Haemorrhage and cerebral damage sustained either during labour and delivery or in the early neonatal period.
d. Necrotizing enterocolitus.
From NEONATAL NEUROLOGY page 139, we are told that ” Levene and Starte (1981) studied 202 consecutive admissions of all birth weights, 68 (34%) of whom were found to have intracranial haemorrhage”
From NEONATAL NEUROLOGY page 76, we are told that approx. 27% of premature infants born in the 31st to 34th weeks develop Periventricular haemorrhages.
From NEONATAL NEUROLOGY ,page 63, we are told that approx. 7% of premature infants born with a birth weight of 1.8 kilograms or less have subarachnoid haemorrhage.
From NEONATAL NEUROLOGY page 57, we are told that ” Intracranial haemorrhage occurs commonly in newborn infants and is an important cause of death & handicap.”
It is evident therefore, that brain haemorrhages in infants is common.
It is also a well documented fact that due to the lack of development of the blood vessels the premature infant is at an increased risk of haemorrhage.
Subdural Haematomas.
From NEONATAL NEUROLOGY, page 58, we are told that “the cause of this type of condition is usually traumatic, that the incidence of it has greatly reduced over recent years and that It has not however, completely disappeared; indeed it may still be a relatively common lesion affecting the neonatal brain and may be associated with few clinical signs, thus remaining undiagnosed during life.”
I need to tidy up the following two graphics and information on originators. Brian.
Note the difference between the following two sets of statements referring to the cause of subdural haemorrhages.

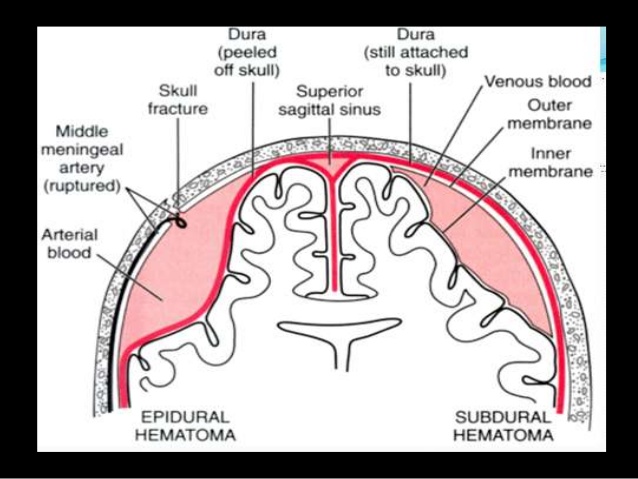
 The first is a bit confusing (like most medical literature) but I read this as 1. Actual damage to the head. 2. Caused by distortion of the brain during the birth process.
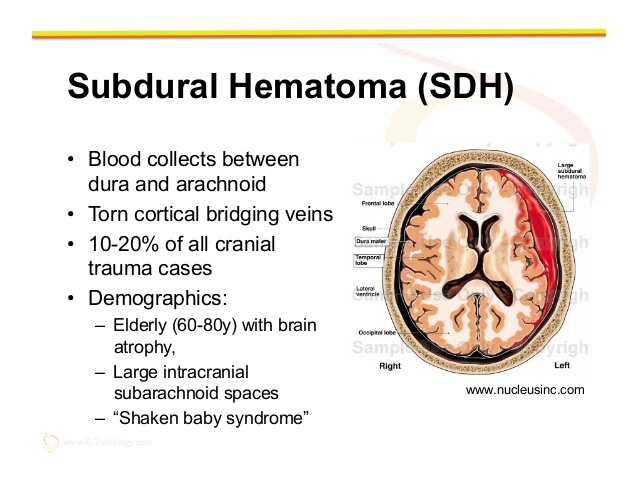
The first is a bit confusing (like most medical literature) but I read this as 1. Actual damage to the head. 2. Caused by distortion of the brain during the birth process.The second set of statements is also slightly confusing, but I read this as “Blood collects between the dura and arachnoid layers, due to torn veins. Subdural Haematomas comprise 10 – 20% of all cranial trauma cases.
The three main causes of the torn veins is 1. Brain atrophy in the elderly. 2. Large intracranial subarachnoid spaces.
3. “Shaken Baby Syndrome”.
Relating to demographics, it should read. 1. Elderly people with brain atrophy. 2. People with large intracranial subarachnoid spaces. 3. “Shaken Baby Syndrome” is not a demographic type.
There can be many causes of subdural haemotomas to people who are not between the ages of 60-80 with brain atrophy, or people who have large intracranial subarachnoid spaces.
Falls can occur to people of all ages. Are the paediatricians really asking us to believe, that subdural Haematomas only happen to the people mentioned in the above two demographic categories plus babies that are shaken or thrown about? If a 30year old man falls off a ladder, are the paediatricians saying that the man cannot suffer from a subdural Haematomas due to falling?
In the drawing below there are numerous large and small veins shown. During the birth process the head can get quite seriously distorted, because at this stage the skull is quite soft and pliable to enable the head to pass through the birth canal.
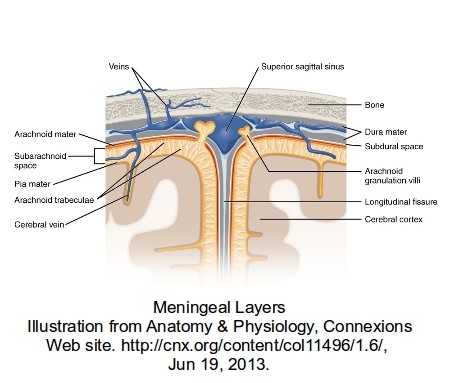 Excluding any accelerations or decelerations (obviously not applicable during the birth process unless the paediatrician is (non-accidentally) shaking the mother or throwing her onto the floor), the main stresses are distortions to the head caused primarily by the natural pressure of the birth process working against the restriction of the birth canal. It should be remembered that the skull is not bone at this stage, and although giving some protection to the brain, is not a crash helmet. In the area of the fontanelle, the very soft area of the skull in babies, the brain is virtually unprotected.
Excluding any accelerations or decelerations (obviously not applicable during the birth process unless the paediatrician is (non-accidentally) shaking the mother or throwing her onto the floor), the main stresses are distortions to the head caused primarily by the natural pressure of the birth process working against the restriction of the birth canal. It should be remembered that the skull is not bone at this stage, and although giving some protection to the brain, is not a crash helmet. In the area of the fontanelle, the very soft area of the skull in babies, the brain is virtually unprotected.Squeezing of the brain tends to to force it forward and bulge into the fontanelle area, but being restrained by the dura-mater. This will cause stretching on the inside of the dura-mater that can damage veins and capillaries that then bleed into the subdural space.
Obviously there are many things to consider; Is it a rapid/easy birth or an extended/complicated birth? Is it a full term baby or premature? How much external handling of the birth was required?
The birth process is not a guaranteed simple process especially in a first birth for the mother. The mother’s natural anxiety with her first birth can complicate the process. The mother’s anatomy can have a great effect on the birth process.
Jaundice Causes
Excess bilirubin (hyperbilirubinemia) is the main cause of jaundice. Bilirubin, which is responsible for the yellow color of jaundice, is a normal part of the pigment released from the breakdown of “used” red blood cells.
Normally, the liver filters bilirubin from the bloodstream and releases it into the intestinal tract. A newborn’s immature liver often can’t remove bilirubin quickly enough, causing an excess of bilirubin. Jaundice due to these normal newborn conditions is called physiologic jaundice, and it typically appears on the second or third day of life.
Other causes
An underlying disorder may cause jaundice. In these cases, jaundice often appears much earlier or much later than physiologic jaundice. Diseases or conditions that can cause jaundice include:
-
Internal bleeding (hemorrhage)
-
An infection in your baby’s blood (sepsis)
-
Other viral or bacterial infections
-
An incompatibility between the mother’s blood and the baby’s blood
-
A liver malfunction
-
An enzyme deficiency
-
An abnormality of your baby’s red blood cells that causes them to break
—————————————
From. wikipedia.org/wiki/Shaken_baby_syndrome/legal issues
In 2012, Dr. A. Norman Guthkelch, the neurosurgeon often credited with “discovering” the diagnosis of SBS,[54] published an article “after 40 years of consideration,” which is harshly critical of shaken baby prosecutions based solely on the triad of injuries.[55] Again, in 2012, Dr. Guthkelch stated in an interview, “I think we need to go back to the drawing board and make a more thorough assessment of these fatal cases, and I am going to bet . . . that we are going to find in every – or at least the large majority of cases, the child had another severe illness of some sort which was missed until too late.”[56] Furthermore, in 2015, Dr. Guthkelch went so far as to say, “I was against defining this thing as a syndrome in the first instance. To go on and say every time you see it, it’s a crime…It became an easy way to go into jail.”[57]
On the other hand, Teri Covington, who runs the National Center for Child Death Review Policy and Practice, worries that such caution has led to a growing number of cases of child abuse in which the abuser is not punished.[54]
This is a rather nasty statement (by Teri Covington) to make. She is implying that irrespective of the evidence, the people charged with SBS are actually the abusers. Brian.
———————————–
More to follow
——————————————
Author; Brian Williams.
-